Bubble contrast echocardiogram (echo
This page is to give you information about your planned bubble contrast echocardiogram.
On this page
-
What is a bubble contrast echocardiogram?
-
Why am I having this test?
-
Why might there be a hole in this part of my heart?
-
What happens if I have a PFO or ASD?
-
Are there alternative reasons to perform the test?
-
What happens during a bubble contrast echo?
-
Do I need to take any special precautions before the test?
-
Is injecting air into the bloodstream harmful?
-
Risks, contra-indications, and side effects
-
After the procedure
-
Contact information
-
Further information
What is a bubble contrast echocardiogram?
You may have already had an echocardiogram (echo) performed. This is a non-invasive and painless imaging test using high frequency sound waves to look at your heart. These frequency sound waves cannot be heard by the human ear. We use it to gain information about the structure and function of the heart, the heart valves, main blood vessels and other structures within the heart. The test does not involve radioactivity (x-rays).
A bubble contrast echo is similar, but during the procedure we will inject ‘microbubbles’ made from saline (sterile salty water). The microbubbles are mixed with a small sample of your blood so that it contains tiny bubbles of air. The bubbles reflect the sound waves and increase the accuracy of the test.
Why am I having this test?
The commonest reason for having this test is because your doctor suspects that you may have a hole in your heart. Most significant holes in the heart are diagnosed in childhood. However, if there is a small defect or hole in the wall (inter-atrial septum) separating the left and right upper chambers of the heart (atria), this may not be found until adulthood. We use the bubble echo to detect these small holes which may not show up on a normal echo.
Why might there be a hole in this part of my heart?
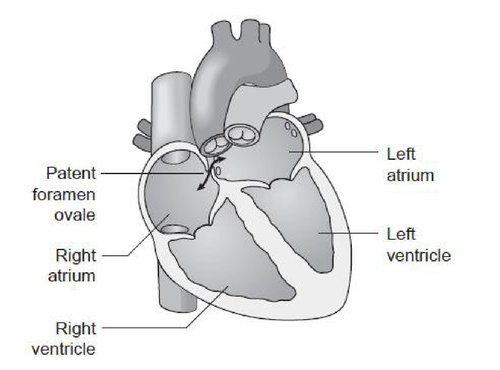
During the normal development of the foetal heart, there is an opening through the inter-atrial septum which allows the circulating blood to bypass the lungs which are not used until birth. Normally, this opening closes in the first few days or weeks after birth, but if it does not, the child will have a communication between the left and right atria.
This may take the form of a hole (Atrial Septal Defect – ASD) or a small channel (Patent Foramen Ovale – PFO) which behaves like a ‘trapdoor’. The defect will often correct itself without any medical intervention before the child reaches the age of 2, but about 25 to 30% of adults in the general population may have a PFO.
What happens if I have a PFO or ASD?
Most people do not have any symptoms or problems because of this defect, and we find it by chance. However, some people may have breathlessness, low blood oxygen or fatigue (tiredness) due to some of the blood circulation bypassing the lungs (known as a shunt). Sometimes, usually when the defect is an ASD, it can lead to enlargement of the right side of the heart.
PFO have also been associated with decompression sickness (the bends) due to the changes in pressure which occur with deep sea diving.
In other people, symptoms can result from blood clots forming in one of the veins in the leg (a deep vein thrombosis – DVT) and then a fragment of clot (embolus) passes from the right to the left side of the heart; this then may block an artery resulting in:
- Stroke (loss of brain function)
- Heart attack (damage to the heart muscle)
Up to 40 to 50% of patients who have had an unexplained stroke, may have a PFO.
Are there alternative reasons to perform the test?
Whilst the commonest reason we do this test is to look for holes in the heart as described on the previous page, we sometimes do this test to investigate patients who have low blood oxygen levels and breathlessness which might also be due to a shunt outside of the heart. Examples may include:
- Extra communications (small holes) between blood vessels in your lungs (known as pulmonary arteriovenous malformations) which may cause the circulating blood to bypass the part of the lungs where oxygen transfers into the blood stream.
- Chronic liver disease which may cause the blood vessels in the lungs to widen and make it harder for your lungs to transfer oxygen to the red blood cells.
What happens during a bubble contrast echo?
- You will be taken into a room with usually a doctor and a cardiac physiologist trained in echocardiography.
- You will be offered a hospital gown, asked to undress to the waist and then lie on a couch. The physiologist will attach ECG stickers to your chest and connect them with wires to the echocardiogram machine. This will monitor your heart rate and rhythm during the test.
- You will have a cannula (small plastic tube) inserted into one of the veins in your arm or hand. This is for the injection of microbubbles. We will then ask you to lie onto your left side. If you are unable to lie on your left side, we can do the echo while you are lying on your back. The test is performed in semi-darkness so the lights will be dimmed once you are comfortable.
- The cardiac physiologist will place the echocardiogram probe on your chest (this is like a thick blunt pen) with cold lubricating jelly (this helps to get good contact with the skin).
- If you have already had an echo, we will go straight on to perform the bubble contrast study. If not, a number of pictures of the heart will be recorded from different areas of your chest. We will then go on to do the bubble contrast study.
- The bubbles are made up in a syringe by rapidly mixing the sterile saline, mixed with a tiny bit of air and some of your blood, drawn back from the vein via the cannula, to make very tiny air bubbles which are then injected through the cannula.
- We will record pictures and watch carefully to see if any bubbles are seen in the left side of the heart.
- We will then ask you to sniff, and you may need to perform a special breathing and blowing technique called the Valsalva manoeuvre. We will explain this technique carefully and allow you to practice before we continue with this part of the test. You do not need to know how to do the Valsalva manoeuvre before you attend. If needed, we will repeat the injections several times.
- The test will take about 30 to 45 minutes to complete. You can return home straight after the test and may drive.
Do I need to take any special precautions before the test?
No, you should take all of your usual medication and can eat and drink normally on the day of the test. We suggest that you keep well-hydrated (having plenty to drink) and keep your hands and arms warm before the test. This increases the chance that we can access a vein for the cannula insertion during the test.
Is injecting air into the bloodstream harmful?
If a large bubble of air was injected into a vein, it could potentially cause harm. However, the air bubbles injected in this test are tiny. If there is no shunt, the lungs will filter out the bubbles.
If you have a shunt, some bubbles will appear on the left side of the heart and then will gradually make their way through the circulation to be filtered out by the lungs.
Risks, contra-indications, and side effects
- The procedure is very safe, and complications are rare.
- The Valsalva manoeuvre involves breathing techniques to changes to the pressure in your chest. This may lead to your ears ‘popping’ or a slight headache.
If you have any ear problems, you should let the doctor know at the start of the test.
- Some people find performing the Valsalva manoeuvre difficult, but we will help you practice as much as we need to and can often still get reasonable images even if the technique cannot be perfected.
- The test does not carry any specific risks. There are no associated allergic reactions with injection of the bubble contrast, so even if you have been allergic to x-ray contrast in the past, that does not stop you having this test.
- If you are taking any blood thinning medication, you may bleed or bruise more easily when we remove the cannula.
After the procedure
Once the test is complete, you can get dressed and are free to leave. We may give you the results immediately, but some findings take longer to interpret and may need a second opinion. The doctor may explain the findings on the day, and a report will be sent to the referring clinician (doctor or specialist nurse).
Contact information
If you have any questions about your planned bubble contrast echocardiogram, please contact:
Cardiac Investigations
Tel: 0300 422 6551
Monday to Friday, 9:00am to 4:00pm
Alternatively, you can contact to your consultant’s secretary through switchboard.
If you would like a chaperone during your procedure, please call and request this in advance. The department will arrange this on your request, as it cannot be a friend or relative, although they may be present if you prefer.